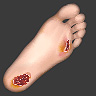
All of us are likely to have problems with our feet but people living with diabetes may develop serious foot problems more quickly and have more complications. In fact, foot problems are one of the leading causes of hospitalization for the 200,000+ British Columbians living with diabetes. About 15% of those with diabetes will develop a serious foot condition at some point in their lives.
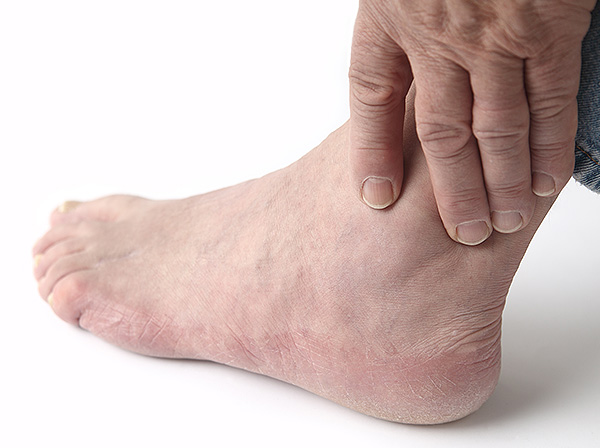
People with diabetes may be at risk for foot-related complications.
Causes of Foot Problems
Diabetic foot problems are usually the result of three primary factors: poor circulation, neuropathy (decreased sensation), and a decreased resistance to infection. Foot deformities and trauma also play major roles in causing ulcerations and infections, particularly when circulation and nerves are impaired.
Poor Circulation
People living with diabetes are at higher risk for developing poor circulation. This often happens as we get older, but complications can occur earlier in life. Chronically tired or painful feet mean circulation is poor. Symptoms such as numbness, tingling, cold or blue feet, and swelling that will not go down, indicate poor circulation. Cramping may occur at night, during rest, or while walking a short distance. Smoking and stress usually increase the severity of these symptoms. An examination by a foot specialist will reveal any circulator deficiencies.
Diabetic Neuropathy
This can cause insensitivity or a loss in the ability to feel pain, heat, and cold. If precautions are not taken, a hot bath can be a potential for a burn. With neuropathy, a person may lose a sense of where their feet are positioned, striking objects in their path. Diabetic neuropathy can also affect the muscles of the feet, causing deformities such as hammertoes. When insensitivity is present, serious problems such as calluses, ulcers, and gangrene can occur without pain. The infection may go unnoticed and appropriate care may be delayed until it is too late. Unfortunately for some diabetic infections, by the time the trouble is discovered, amputation may be necessary to save the person’s life. Daily observation of the feet is necessary by the diabetic, a responsible family member, or medical personnel.
Corns and Calluses
These are build-up of skin that forms at points of pressure or over boney prominences. Corns and calluses can develop into diabetic ulcers. A foot doctor will remove excessive callused skin before it becomes a problem and may suggest changes in foot wear or custom orthotics to relieve the pressure points. People with diabetes should not attempt to remove corns and calluses themselves due to the risk of infection if it is not done properly.
Diabetic Ulcers
They are open sores that can be caused by lack of blood circulation to the foot, lack of soft tissue protection, excessive callus tissue, infection, or pressure points. A diabetic ulcer is a common occurrence with the diabetic foot and should be carefully treated and monitored by a foot specialist.
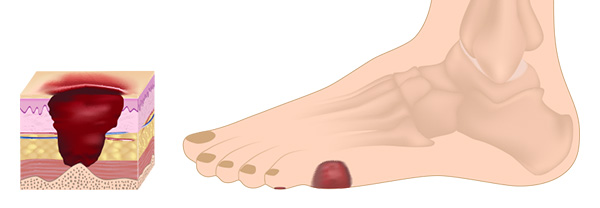
Diabetic ulcerations are common in patients with uncontrolled diabetes and showing symptoms of neuropathy.
Left unattended, such ulcers can quickly become infected and lead to more serious consequences. If the circulatory response is adequate, most diabetic ulcers can be healed if diagnosed and treated early. A foot doctor knows how to help prevent and treat theses wounds to keep your feet healthy and strong.
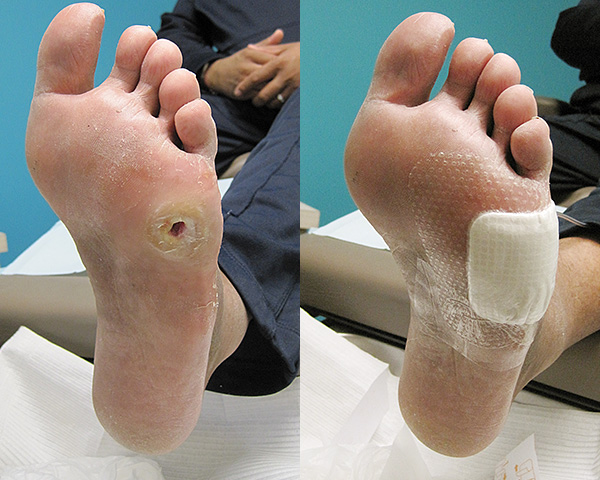
Ulceration in a diabetic patient with lack of sensation to his feet.
Skin Changes
Skin changes in the foot can be caused by diabetes. Dehydration is common since the diabetic usually has less natural lubrication than the non-diabetic. Fissures and cracks in the skin develop and itching can become severe. Scratching can cause breaks in the skin that may become infected. Dryness can be improved by using a good moisturizer daily on every part of the foot except between the toes. A foot doctor can suggest over the counter moisturizer best for your feet or order a prescription strength moisturizer if need be. See the Dry Skin page for more information.
With the potential foot problems that are associated with diabetes, this means you need to take good care of them. Daily inspection of your feet and routine follow up with a foot specialist is important to maintain healthy feet.
What To Do At Home
- Check your feet each day. See a foot specialist (podiatrist) if you notice cuts, sores, or blisters that don’t heal within a few days.
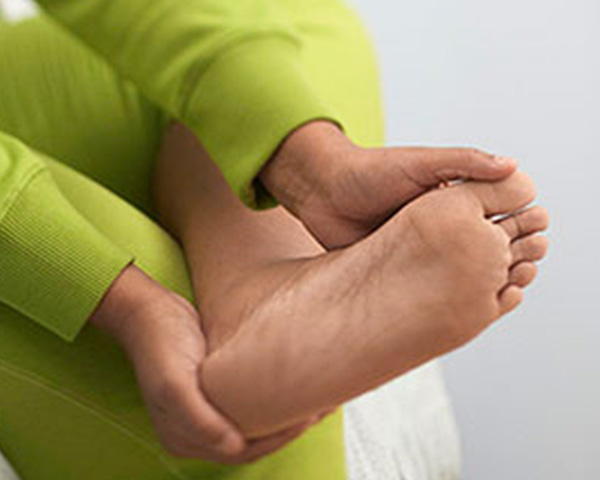
Daily foot checks is essential in preventing diabetes-related foot complications.
- Wash your feet daily in warm (not hot) water. Use a mild soap. Dry well. Be sure to wash and dry between your toes too.
- Use moisturizer each day, best to apply right after shower. This helps prevent dryness and scaling. Don’t put lotion between your toes. See the Dry Skin page for more information.
- Always wear shoes. Change your socks daily. Socks made out of synthetic materials such as acrylic are the best. Avoid cotton socks. Don’t walk barefoot — indoors or outdoors.
- Avoid trimming your toe nails unless instructed by your doctor. For corns and calluses, you should not treat yourself.
Call a foot specialist right away if you notice any of the following:
- Changes in skin colour — redness with streaks is often a sign of infection. Darkened skin may mean the tissue has died. Pale or blue skin may mean poor blood flow.
- Drainage, bleeding or odour — white or yellow moisture, bleeding, or odor are signs of infection or dead tissue.
- Increase in swelling — a swollen foot may be a sign of infection or poor blood flow.
- Temperature changes — warm spots may mean the foot is infected. Cold feet can be a sign of poor blood flow.
- Changes in sensation — numbness, burning, tingling, or lack of feeling may mean nerves are damaged.
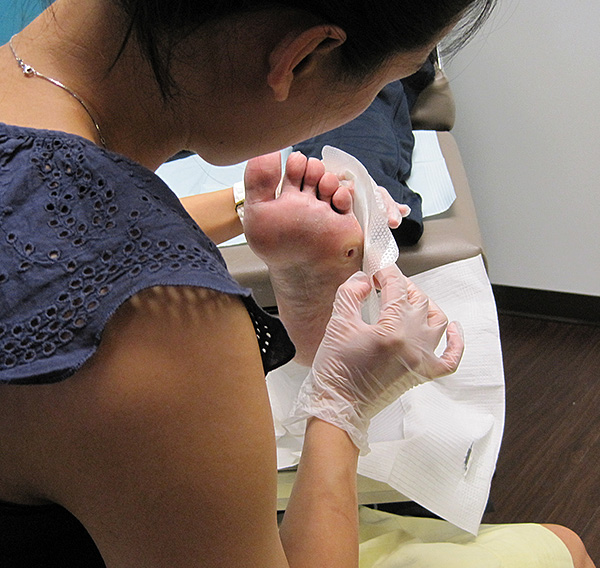
Dr. Alice Wang performing wound care for a patient with diabetic ulcer. Routine visits to a foot specialist is crucial in preventing diabetic foot infections.
Exercises for your feet
Exercise helps keep blood flowing to your feet. It also helps keep your feet more flexible. Walk often. Walking improves blood flow to your feet. It is also good for your general health. Spell out the alphabet in the air with each foot. Do this once a day to help keep your feet flexible.
Wear comfortable shoes and socks
Shoes and socks that fit right help prevent foot problems. They can also help keep any foot problems you have from getting worse.
- Wear shoes that cover your toes and heels.
- Choose shoes with a wide and deep toe box Choose synthetic socks.
- Avoid cotton socks which can retain moisture. It also loses its shape and elasticity more easily, causing friction between your foot and the sock.
- Check your feet after wearing a new pair of shoes. Red spots or blisters are signs that shoes are rubbing or pressing on the foot.
If you or a family member have diabetes or experiencing any of the signs and symptoms described above, it is important to have a foot specialist perform a foot check and suggest long term care to avoid complications. Contact our office for a consultation with Dr. Wang today!