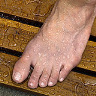
Athlete’s foot is a skin condition caused by a fungus, usually occurring between the toes and bottom of the foot. The fungus most commonly attacks the feet because shoes create a warm, dark, and humid environment which encourages fungus growth. The warmth and dampness to areas around swimming pools, showers, and locker rooms are also breeding grounds for fungi.
Not all fungus conditions are athlete’s foot. Other conditions, such as disturbances of the sweat mechanism, reaction to dyes or adhesives in shoes, eczema, and psoriasis, may mimic athlete’s foot.
Symptoms
The signs of athlete’s foot include dry skin, itching, scaling, inflammation, and blisters. Blisters often lead to cracking of the skin. When blisters break, small raw areas of tissue are exposed, causing pain and swelling. Itching and burning may increase as the infection spreads.
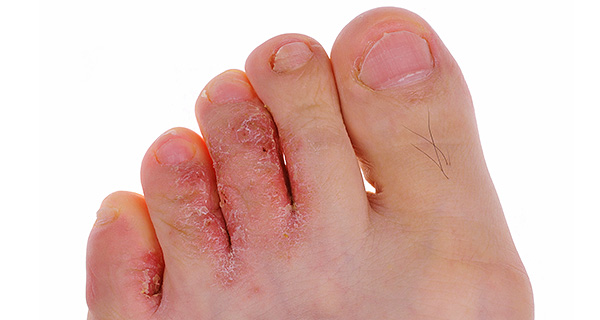
Athlete’s foot can cause dry, itchy, cracked skin in between the toes.
Athlete’s foot may spread to the soles of the feet and to the toenails. It can be spread to other parts of the body, notably the groin and underarms, by those who scratch the infection and then touch themselves elsewhere. The organisms causing athlete’s foot may persist for long periods. Consequently, the infection may be spread by contaminated bed sheets or clothing to other parts of the body.
Prevention

Avoid going barefoot in public areas such as dressing rooms and public showers.
It is not easy to prevent athlete’s foot because it is usually contracted in dressing rooms, showers, and swimming pool locker rooms where bare feet come in contact with the fungus. However, you can do much to prevent infection by practicing food foot hygiene. Daily washing of the feet with soap and water; drying carefully, especially between the toes; and changing shoes and hose regularly to decrease moisture, help prevent the fungus from infecting the feet. Also helpful is daily use of a quality foot powder.
Tips:
- Avoid walking barefoot — use shower sandals.
- Reduce perspiration by using foot powder.
- Wear light and airy shoes.
- Wear socks that keep your feet dry and change them frequently if you perspire heavily. Avoid cotton socks. Synthetic materials such as acrylic wicks away moisture better than cotton.
Treatment
Over the counter medications and creams for athlete’s foot frequently fail to resolve the condition. Prescribed topical or oral drugs are much more effective. In mild cases of the infection it is important to keep the feet dry by dusting foot powder in shoes and hose. The feet should be bathed frequently and all areas around the toes dried thoroughly.
Consult with a foot specialist if an apparent fungus condition does not respond to proper foot hygiene and self care, and there is no improvement within 2 weeks. The doctor will determine if a fungus is the cause of the problem. If it is, a specific treatment plan, including the prescription of anti-fungal medication, applied topically or taken by mouth, will usually be suggested. If the infection is caused by bacteria, antibiotics, such as penicillin, that are effective against a broad spectrum of bacteria may be prescribed.